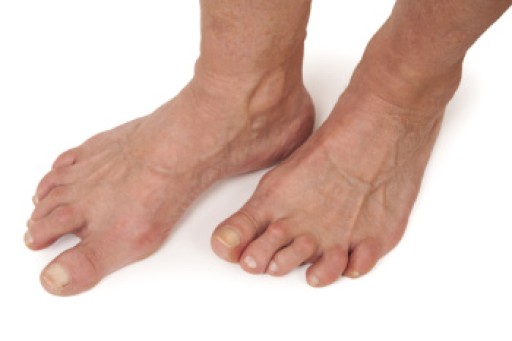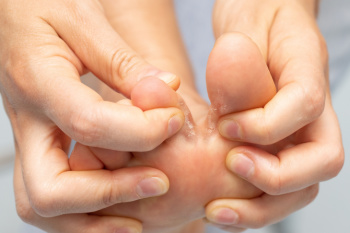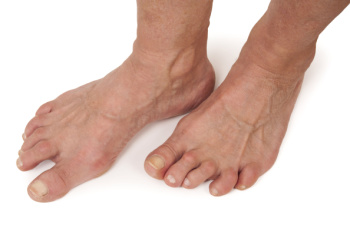
Rheumatoid arthritis, also known as RA, is a prevalent inflammatory condition, affecting up to one percent of the global population. It can develop at any age but is most common in individuals that are between 30 and 50 years old, with significant disability implications. Genetic factors play a substantial role, with approximately half the risk attributable to genetic predisposition, including specific human leukocyte antigen associations. Smoking is a major environmental trigger. RA primarily affects joints, leading to synovial inflammation, cartilage damage, and bone erosion. Symptoms include joint pain, stiffness, and swelling, often affecting the toes of the feet. Morning stiffness lasting over an hour is a hallmark sign. If you have discomfort in your feet from RA, it is suggested that you schedule an appointment with a podiatrist, as prompt diagnosis is essential for early intervention and management to mitigate joint damage and preserve joint function.
Because RA affects more than just your joints, including the joints in your feet and ankles, it is important to seek early diagnosis from your podiatrist if you feel like the pain in your feet might be caused by RA. For more information, contact one of our podiatrists of Biebel & DeCotiis Podiatry Associates. Our doctors will assist you with all of your podiatric concerns.
What Is Rheumatoid Arthritis?
Rheumatoid Arthritis (RA) is an autoimmune disorder in which the body’s own immune system attacks the membranes surrounding the joints. Inflammation of the lining and eventually the destruction of the joint’s cartilage and bone occur, causing severe pain and immobility.
Rheumatoid Arthritis of the Feet
Although RA usually attacks multiple bones and joints throughout the entire body, almost 90 percent of cases result in pain in the foot or ankle area.
Symptoms
- Swelling and pain in the feet
- Stiffness in the feet
- Pain on the ball or sole of feet
- Joint shift and deformation
Diagnosis
Quick diagnosis of RA in the feet is important so that the podiatrist can treat the area effectively. Your doctor will ask you about your medical history, occupation, and lifestyle to determine the origin of the condition. Rheumatoid Factor tests help to determine if someone is affected by the disease.
If you have any questions please feel free to contact one of our offices located in Holmdel and Middletown, NJ . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.